Overview
Bilateral cataracts are a common eye disorder characterized by the formation of cloudy areas in the lenses of both eyes. The prevalence of bilateral cataracts increases with age. In people over the age of 65, it is estimated that 70% have bilateral cataracts.
Globally, cataract is the leading cause of blindness. It is estimated that there are 253 million people in the world who are blind or visually impaired due to cataract. In low- and middle-income countries, cataract is the leading cause of blindness in people over the age of 50.
Let’s take a look at what bilateral cataracts are.
What is a Bilateral Cataract?
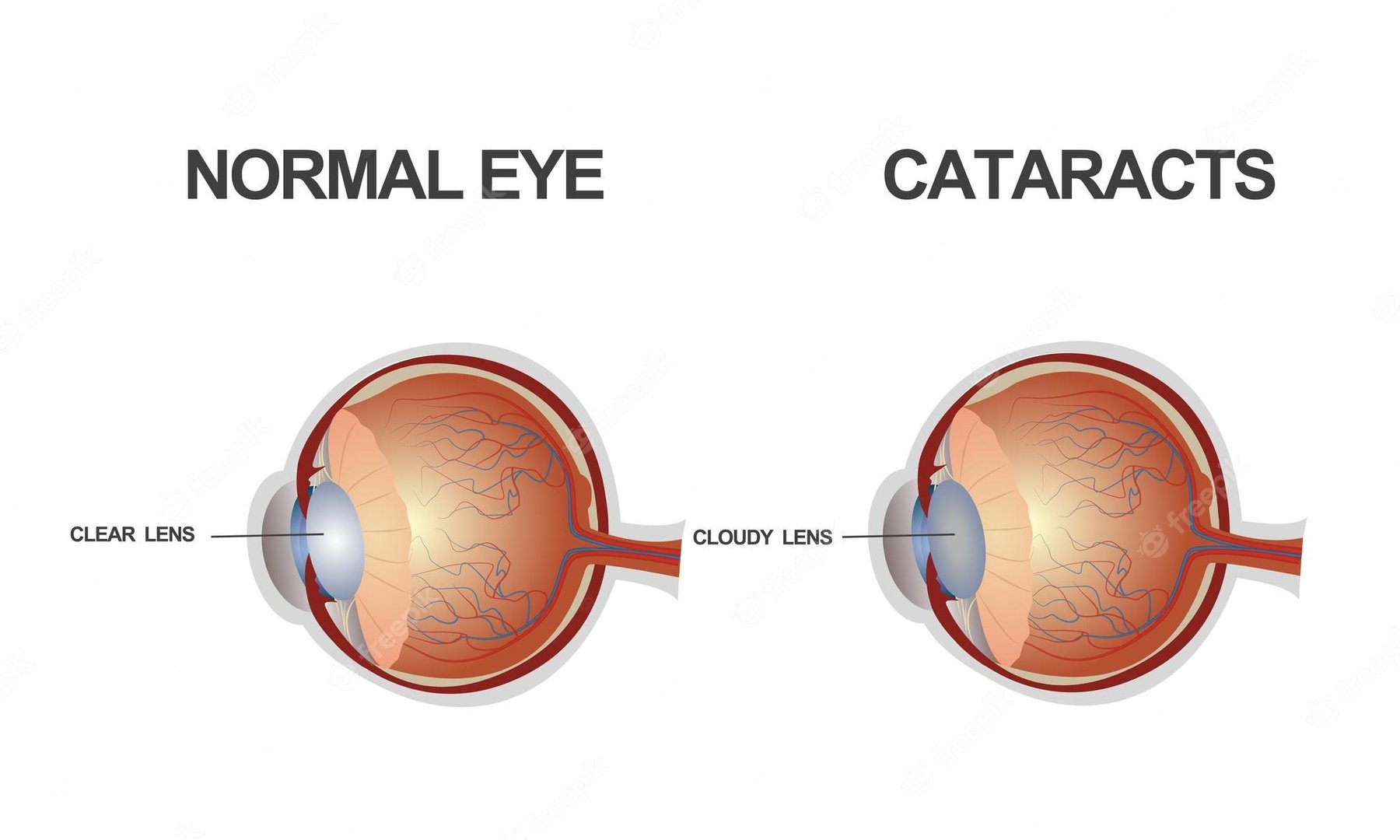
Cataracts are a prevalent eye condition that occurs when the lens of the eye becomes cloudy. It leads to blurry vision and impaired eyesight. When cataracts develop in both eyes simultaneously or at different times, they are referred to as bilateral cataracts.
Cataracts can cause blurry or impaired vision, which makes it difficult to read, drive, or recognize faces.
The good news is that cataracts are treatable with a quick procedure that swaps out the hazy lens for an artificial one that is clear. This procedure is risk-free and productive, restoring eyesight clarity while improving quality of life.
Wondering what causes bilateral cataracts? Let’s explore.
Take charge of your health with the best treatment. Book your consultation now.
What Causes Bilateral Cataracts?
Bilateral cataracts are usually the result of a combination of factors. These factors include aging, genetic predisposition, exposure to ultraviolet (UV) light from the sun, as well as specific medical conditions like diabetes. These factors can lead to the clouding of the eye's natural lens over time, affecting both eyes.
Aging is the most frequent cause of cataracts. Age-related protein breakdown and protein clumps in our eye lenses can cause cloudiness and decreased vision.
- Genetics:
The influence of heredity can be felt. You can be more prone to acquiring cataracts if the condition runs in your family.
- Medical Conditions:
Diabetes and other metabolic diseases, for example, can raise the chance of cataract formation.
- Trauma or Injury to the Eye:
Eye trauma or injuries can harm the lens of the eye and cause cataracts.
- Long-term Sun Exposure:
Prolonged exposure to the sun's ultraviolet (UV) rays can raise your chance of developing cataracts.
- Drug:
Corticosteroids are one type of drug that can hasten the development of cataracts.
- Alcohol and Smoking:
Smoking and binge-drinking have both been linked to an increased risk of bilateral cataract.
- Previous eye operations:
A few eye operations or prolonged contact lens wear may raise the incidence of cataracts.
Apart from that, some medications and eye injuries can also contribute to the development of cataracts. If you suspect you have cataracts or have concerns about your eye health, it's important to consult with an eye specialist for a proper evaluation and treatment options.
What are you thinking? How to identify whether you have bilateral cataracts or not?
Let’s find out the signs of bilateral cataracts.
How Do I Know if I have Bilateral Cataracts?
It's conceivable that you have bilateral cataracts if you're displaying specific vision-related symptoms. Typical signs include:
Blurry Vision:
Vision becomes clouded or fuzzy as if being seen through a foggy or frosted window.
Reduced Night Vision:
The inability to see in lit environments, such as at night or during the day.
Sensitivity to Light:
More sensitive to glare and bright lighting.
Colors Appearing Fade:
Colors may seem faded or less bright.
Double vision:
It is the perception of two or more images in one eye.
Frequent Prescription Changes:
Need regular adjustments to your prescription for glasses or contact lenses.
Halos Around Lights:
Observing rings or halos around lights, particularly in lit areas.
Reading or Close-Up Work Difficulties:
Have trouble reading, stitching, or carrying out chores that call for sharp close-up eyesight.
It's crucial to arrange an eye checkup with an optometrist or ophthalmologist if you're exhibiting one or more of these symptoms. To learn whether bilateral cataracts are the root of your problems, they may conduct a thorough eye examination that may include visual acuity tests, eye health evaluations, and other diagnostic exams.
Let's take a look at the solutions for bilateral cataracts.
Can Bilateral Cataracts Be Treated?

Yes, it is possible to treat bilateral cataracts. Surgery is the main form of care for cataracts where doctors can perform bilateral cataract removal. The normal lens of the eye is removed during cataract surgery and is replaced with an intraocular lens (IOL), an artificial lens. This technique has a high success rate for restoring eyesight clarity and is generally safe.
An outline of the bilateral cataract surgery procedure is provided below:
- Preoperative Evaluation:
To determine the severity of your cataracts and your eye health, your eye specialist will conduct a thorough eye examination. The best treatment strategy is chosen with the aid of this examination.
- Surgery:
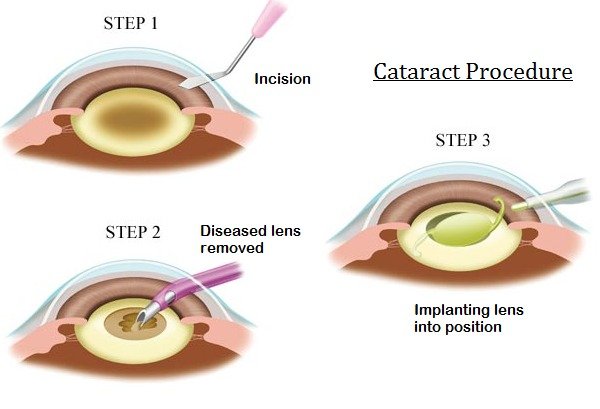
A small incision is made in the eye during cataract surgery. Through the use of methods like phacoemulsification, the clouded lens is dispersed and eliminated. Then, to restore vision, a synthetic IOL is placed in its place.
- Recovery:
Since cataract surgery is performed as an outpatient operation, recovery is usually not too long. After bilateral cataract surgery most patients see an improvement in their eyesight within a few days to weeks.
- Follow-up Care:
Your eye doctor will schedule follow-up visits with you to check on your recovery and make sure your eyes are healing.
- Vision Correction:
You may select a basic monofocal IOL. It corrects vision for one distance (often distance vision), based on your preferences and eye health, or a premium IOL. This can correct vision for many distances, lowering the need for glasses.
Cataract surgery is very effective at restoring vision, and many patients report that their eyesight and quality of life have improved. But there are potential dangers and complications, like with any surgical procedure. Before the procedure, your eye doctor will go over these issues with you.
Are you worried about the safety of cataract surgery? Then read ahead to learn more.
Is Cataract Surgery Safe?
Yes, cataract surgery is regarded as a common, safe technique with a high rate of success. Most cataract operations are carried out without incident, and patients report considerable improvements in their vision and quality of life as a result.
Over time, improvements in technology, anesthetic, and surgical methods have made cataract surgery both safer and more productive. Since the procedure is often done as an outpatient, you won't need to spend the night in the hospital.
Although they are uncommon, cataract surgery does have possible risks and problems, like any other medical procedure. Potential risks include:
- Infection:
There is a slight chance of infection, which, if discovered, is treatable with antibiotics.
- Swelling or Inflammation:
Temporary edema or inflammation of the eye may occur in some patients.
- Bleeding:
Minor bleeding during surgery is possible, but it's usually controllable.
- Retinal Detachment:
The retina, which is the light-sensitive tissue at the back of the eye, can separate following surgery, necessitating rapid medical intervention.
- Glaucoma:
Glaucoma, a disorder that damages the visual nerve, can be brought on by or made worse by cataract surgery.
- Corneal edema:
An accumulation of fluid in the cornea may happen, impairing vision.
Before the procedure, your doctor will go over these possible risks with you and check your personal risk factors. To reduce any potential difficulties, it's crucial to provide your doctor a thorough medical history and adhere to all preoperative and postoperative instructions.
After a comprehensive examination of your eye health and general well-being, your eye care professional should help you decide whether to have cataract surgery. They can offer you individualized advice and support you in coming to a choice based on your particular circumstances.
Is it a myth that cataracts might return after surgery? Let’s check ahead.
Take the first step to recovery. Get in touch with us for your treatment.
Can Cataracts Come Back After Surgery?
No, once a cataract has been removed during surgery, it cannot grow back.
Yet, a condition called "posterior capsule opacification" or "secondary cataract" can induce symptoms comparable to blurred vision. The posterior capsule, a slender, transparent membrane that holds the artificial intraocular lens (IOL) in place, becomes clouded over time, which causes this to happen.
This posterior capsule clouding may cause symptoms including hazy or fuzzy vision, which are comparable to those of a cataract. It's crucial to understand that this is not the same as the original cataract coming back.
The "YAG laser capsulotomy" is a rapid and painless laser surgery that is helpful for treating this issue. The hazy posterior capsule is opened during this technique, enabling vision to be seen.
It's important to note that posterior capsule opacification is not a common side effect of cataract surgery. The risk differs from person to person and can be affected by elements including the kind of IOL utilized and unique healing processes.
It's crucial to talk to your eye doctor if your eyesight changes after cataract surgery. If needed, they can recommend the appropriate treatment after assessing whether the changes are caused by posterior capsule opacification or other factors.
From surgery to clear vision: Navigating recovery time.
How Long Does it Take to Recover from Cataract Surgery?

After cataract surgery, the recovery period is brief, and the majority of patients notice noticeable improvements in their vision within a few days to weeks. Here is a broad timeline of things to anticipate during recovery:
After a procedure:
- You'll stay in a recovery area for a short while after the operation to make sure you're recovering well.
- Tearing, light sensitivity, and minor discomfort are possible, but these symptoms often go away soon.
Initial Days:
- During the first few days, it's normal to notice some minor blurriness, shifting vision, or haziness.
- To stop infection and promote healing, you must use the eye drops your doctor has recommended.
Initial Week:
- Within the first week, many patients report increased vision
- Even at night, you might still experience some light sensitivity, glare, or halos surrounding lights.
Weeks 2-4:
- As your eye heals, your vision gets better and better.
- Most patients have improved eyesight by the end of the first month and may resume the majority of normal activities.
Further to that:
- It may take several months for a full recovery.
- During this time, you can find that your vision becomes more stable and clear.
For certain people, activities like reading or driving may need the use of glasses.
It's crucial to follow your doctor's post-operative recommendations. This can includes
- taking the eye drops that have been given
- Avoiding strenuous activities.
- shielding your eyes from direct sun rays and
- Going to follow-up appointments to check on your recovery.
Take a look on the steps to keep bilateral cataracts at bay.
Is There Any Way to Prevent Bilateral Cataracts?
There isn't any particular technique to stop bilateral cataracts from developing. But there are several lifestyle choices and preventative measures that may help lower the risk or delay their beginning. Here are some actions you might want to take:
- Protect Your Eyes from UV Radiation:
Cataracts can develop as a result of prolonged sun exposure to ultraviolet (UV) rays. When you're outside, use sunglasses that filter UVA and UVB rays, and think about donning a wide-brimmed hat for extra protection.
- Stop Smoking:
Smoking has been associated with an increased chance of developing cataracts.
- Maintain a Healthy Diet:
Consuming an anti-inflammatory, vitamin and mineral-rich diet can improve eye health. Eat things like leafy greens, colorful fruits and vegetables, and omega-3 fatty acids.
- Manage Medical Conditions:
Certain health issues, such as diabetes and high blood pressure, might make cataracts more likely. To help reduce the risk, treat these conditions as needed.
- Stay Active:
Engaging in regular physical activity and maintaining a healthy weight can improve eye health by improving wellbeing.
- Stay Hydrated:
Drink enough water to keep your body hydrated, which includes your eyes.
- Limit Your Alcohol Consumption:
Drinking too much alcohol has been linked to an increased risk of cataracts. Modesty is important.
- Regular Eye Exams:
Scheduling regular comprehensive eye exams is of utmost importance. It will help your doctor to find if any early indications of cataracts and offer advice on how to take care of your eye health.
- Eye Protection:
Wear the proper eye protection if you engage in any activity that could result in eye injury, such as sports or certain professions.
- Manage Your Medications:
Corticosteroids, in particular, can raise your risk of developing cataracts. If you use a long-term medicine, talk to your doctor about any potential hazards.
While taking these precautions can help maintain healthy eyes, it's vital to keep in mind that cataracts are a normal part of aging. Making regular eye examinations and consulting with an eye care specialist is crucial if you want to preserve your eye health and receive expert guidance. This is even more important if you're at risk or experiencing any vision issues.
Your health is too important to ignore – schedule your appointment now.
References:
https://cataracteyesurgery.co/types/bilateral-cataracts/
https://www.nhs.uk/conditions/cataract-surgery
https://www.reviewofophthalmology.com/article/two-for-one-bilateral-cataract-surgery